Table of Contents
Infected ingrown hair removal requires checking warning signs first. Look for spreading redness, warmth, pus, or red streaks. Normal bumps stay small and soft. Infected tissue feels hard and throbs. Treat minor cases at home with warm compresses 3-4 times daily. Apply antibiotic ointment. Extract only when the hair tip shows using sterilized tools. Never squeeze or dig deep. Stop home treatment and see a doctor for fever, red streaks, or areas larger than two inches. High-risk patients need care within 24 hours. Doctors prescribe antibiotics or drain abscesses. Prevent future infections by shaving with hair growth using fresh blades. Exfoliate daily with salicylic acid. Wear loose cotton clothing. Choose laser or electrolysis to permanently stop recurring cycles.
Question | Answer |
|---|---|
How can I tell if an ingrown hair is infected? | Infected ingrown hairs display spreading redness, warmth, yellow pus, and red streaks while normal bumps remain small, soft, and painless. |
When should I see a doctor for an infected ingrown hair? | Seek immediate medical care if you develop fever, notice red streaks spreading from the site, or the area exceeds two inches in size. |
Can I remove an infected ingrown hair at home? | Attempt home removal only when the hair tip is visible or a whitehead has formed, using sterilized tools after warm compresses. |
How do I prevent ingrown hairs from becoming infected? | Prevent infections by shaving with hair growth direction, exfoliating daily with chemical acids, and wearing loose cotton clothing after removal. |
What permanently stops recurring infected ingrown hairs? | Laser hair removal and electrolysis permanently destroy follicles to eliminate recurring infected ingrown hair cycles. |
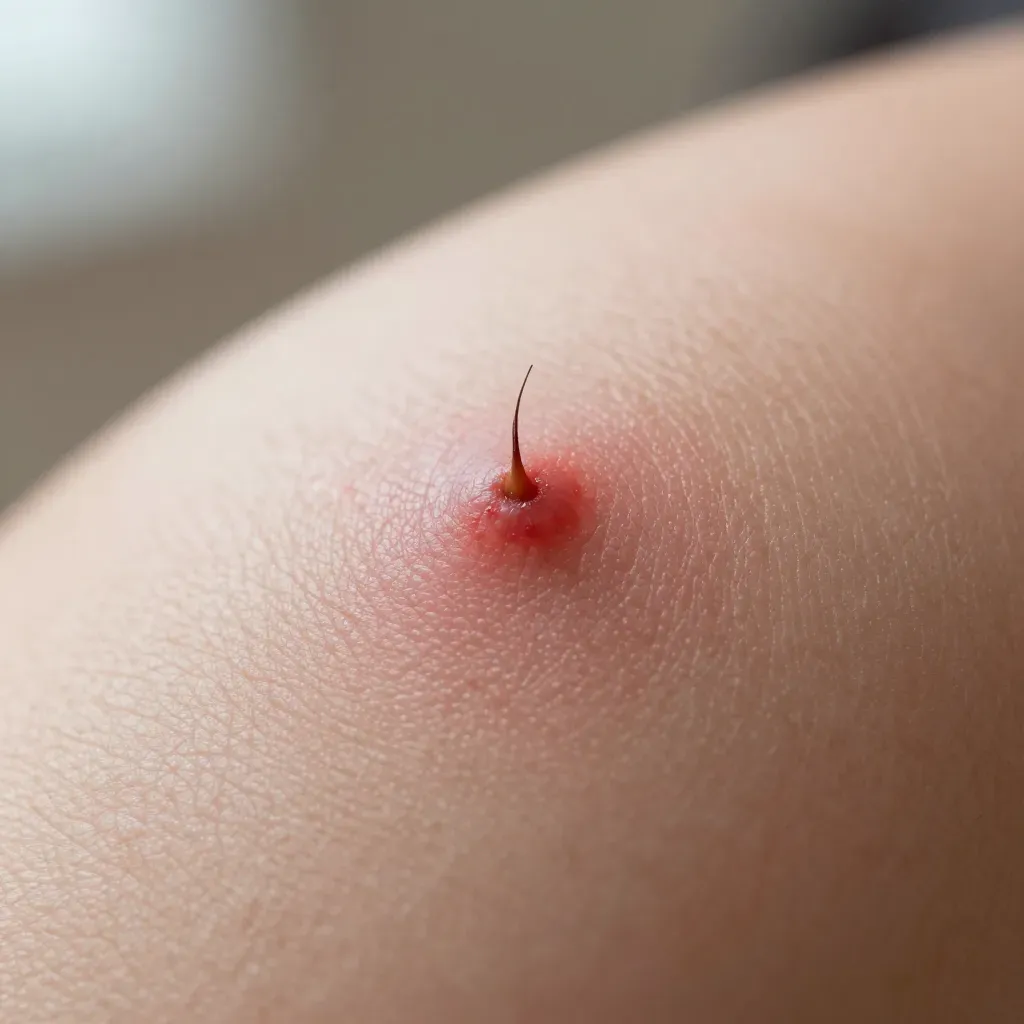
Recognize the warning signs of an infected ingrown hair before attempting removal.
Infected ingrown hair removal requires careful assessment first. Normal ingrown hairs show small red bumps. Infected ones display spreading redness, warmth, and yellow pus.
Visual differences between normal and infected bumps
Normal ingrown hair | Infected ingrown hair |
|---|---|
Small red bump | Expanding red area |
Mild tenderness | Throbbing pain |
No drainage | Yellow or green pus |
Skin color normal around bump | Red streaks spreading outward |
Soft to touch | Hard, fixed swelling |
Warning signs that demand medical attention
- Fever or chills accompany the bump
- Red streaks travel away from site
- Area feels hot to touch
- Pus drains continuously
- Swelling doubles size within 24 hours
- Skin turns dark red or purple
- Foul or metallic odor present
Check the area size. Infections larger than a quarter inch usually need antibiotics. Small localized pus pockets sometimes drain naturally. Wait 48 hours before attempting any extraction. Early stage infections respond to warm compresses. Advanced infections require prescription treatment.
Texture and sensation indicators
Press gently around the bump. Normal tissue feels soft and moves easily. Infected tissue feels hard, fixed, and produces sharp pain with pressure. The skin may crack or weep clear fluid before pus emerges. Folliculitis often clusters multiple infected hairs together. Abscess formation creates a pocket of pus beneath the skin surface.
Apply safe at-home treatments to reduce inflammation and draw out the trapped hair.
Warm compress protocol
Apply warm compresses 3-4 times daily. Use clean washcloth soaked in hot water. Press against bump for 10-15 minutes. Heat dilates pores and draws pus toward surface. Repeat until whitehead forms or hair tip emerges.
Topical treatments
Treatment | Application | Frequency |
|---|---|---|
Antibiotic ointment | Thin layer on clean skin | 2-3 times daily |
Drawing salve | Cover with bandage | Overnight |
Tea tree oil | Diluted 1:10 with carrier oil | Once daily |
Hydrocortisone cream | Reduce inflammation only | Twice daily, max 3 days |
Safe extraction technique
Only extract when hair tip visible or whitehead present. Sterilize needle with alcohol. Pierce surface gently parallel to skin. Do not dig deep. Use tweezers to pull hair straight out. Stop if bleeding or severe pain occurs. Apply antibiotic ointment immediately after.
What to avoid
- Squeezing or popping before ready
- Unclean tools
- Deep digging with needles
- Depilatory creams on broken skin
- Tight clothing friction
Know when to stop home treatment and seek medical care for infected ingrown hairs.
Timeline limits for home treatment
Stop home treatment after 3-5 days without improvement. Worsening symptoms within 48 hours demand immediate medical evaluation. Persistent pain despite warm compresses indicates deeper infection requiring antibiotics.
Critical warning signs
Symptom | Action required |
|---|---|
Fever over 100.4°F | ER or urgent care within 4 hours |
Red streaks (lymphangitis) | Same-day medical appointment |
Area larger than 2 inches | Doctor visit within 24 hours |
Throbbing pain unrelieved by OTC meds | Immediate evaluation |
Black or gray skin discoloration | Emergency department |
Pus drainage lasting over 3 days | Medical assessment needed |
High-risk conditions
- Diabetes or prediabetes
- Immunocompromised status (HIV, chemotherapy, steroids)
- History of MRSA infections
- Blood circulation disorders
- Facial triangle infections (nose/upper lip)
Medical interventions available
Doctors perform incision and drainage for abscesses. Oral antibiotics treat cellulitis. Culture tests identify resistant bacteria like MRSA. Surgical excision removes chronically infected follicles. Professional removal prevents recurrence in problematic areas.
Prevent future infections by changing hair removal habits and skin care routines.
Modify shaving technique
Shave with hair growth direction, never against. Use single-blade razors or electric trimmers. Replace blades every 5-7 uses. Soak skin in warm water 3 minutes before shaving. Apply shaving gel. Never dry shave.
Exfoliation protocol
Exfoliate 24-48 hours before hair removal. Use chemical exfoliants (salicylic acid 2%, glycolic acid) instead of harsh scrubs. Daily gentle chemical exfoliation prevents dead skin buildup that traps hairs.
Post-removal care routine
- Rinse with cool water immediately
- Apply fragrance-free moisturizer within 3 minutes
- Avoid touching or picking skin for 24 hours
- Wear loose cotton clothing
- Skip workouts for 24 hours to prevent sweat friction
Clothing and friction management
Tight synthetic fabrics trap bacteria and force hairs backward. Switch to breathable cotton underwear. Change out of sweaty clothes within 30 minutes. Avoid tight jeans or leggings immediately after shaving.
Removal method | Infection risk | Prevention strategy |
|---|---|---|
Waxing | High | Verify sterile equipment, avoid broken skin |
Shaving | Medium | Fresh blade, shave with grain only |
Depilatory creams | Low | Patch test first, rinse thoroughly |
Laser/IPL | Very low | Follow pre/post protocols strictly |
Consider alternative hair removal methods if shaving constantly causes infections. Laser treatments destroy follicles permanently and eliminate ingrown hair cycles entirely.
Explore professional removal options for recurring infected ingrown hairs.
Dermatological extraction
Dermatologists perform sterile extraction under local anesthesia. They lance abscesses and remove hair fragments with sterile needles. This resolves acute infections but does not prevent future occurrences.
Laser hair removal
Laser destroys follicles permanently and stops the ingrown cycle. Diode lasers treat most skin types. Nd:YAG lasers work for darker skin tones. Professional laser systems require 6-8 sessions for complete clearance. Results last years or permanently.
Electrolysis
Electrolysis inserts a probe into each follicle to destroy growth cells. Works on all hair colors including blonde and gray. Electrolysis for ingrown hairs suits small areas like the chin or bikini line where lasers struggle.
Medical treatments for chronic cases
Treatment | Best for | Duration |
|---|---|---|
Oral antibiotics | Recurring folliculitis | 2-4 weeks |
Retinoid creams | Follicle blockage prevention | Ongoing |
Steroid injections | Keloid scars from infections | Monthly sessions |
Prescription washes | Bacterial colonization | Daily use |
When to choose professional over home care
Seek professional options after three or more infections in the same area within six months. Professional versus at-home devices differ significantly in power and safety for infected areas. Medical intervention prevents scarring and hyperpigmentation from repeated home extraction attempts.